Table of Contents
Understanding Ozempic and Diverticulitis Concerns
With Ozempic gaining widespread attention for managing type 2 diabetes and supporting weight loss, many wonder: can you take Ozempic if you have diverticulitis? This question arises as millions in the US turn to this medication, but those with gastrointestinal histories face unique worries. About 50 million adults deal with diverticulitis or related issues, making it essential to explore how GLP-1 agonists with gut issues might intersect.
Ozempic, known generically as semaglutide, acts as a GLP-1 receptor agonist. It mimics hormones that slow gastric emptying, much like a traffic controller easing food through the digestive tract to regulate blood sugar levels. This mechanism helps control diabetes and promotes satiety for weight management. Over 1.7 million prescriptions occur monthly in the US, yet its effects on digestion prompt caution for sensitive conditions. According to Healthline, up to 20% of users experience gastrointestinal side effects, highlighting why semaglutide and colon inflammation deserve attention.
Diverticulitis involves inflammation of small pouches, or diverticula, forming in the colon wall. Common in people over 60, it affects roughly 30% of those in their 50s and rises to 60% by age 80 in the US. Symptoms include abdominal pain, bloating, fever, and changes in bowel habits, often flaring from infection or blockage. For those managing this, any medication altering gut motility raises red flags.
Addressing these overlaps, Does Ozempic Affect Diverticulitis becomes a key consideration, alongside risks like ozempic gastroparesis or ozempic pancreatitis. Upcoming sections delve into fundamentals, potential interactions, and advice. Always consult your healthcare provider before starting, as this overview does not replace professional medical guidance.
Ozempic Basics and Diverticulitis Fundamentals
Ozempic, known generically as semaglutide, is a GLP-1 receptor agonist medication primarily used to manage type 2 diabetes and support weight loss. It works by mimicking incretin hormones, which signal the pancreas to release insulin after meals while suppressing glucagon, helping to regulate blood sugar levels effectively. For those wondering, can you take ozempic if you have diverticulitis, the answer hinges on individual health profiles and potential gastrointestinal interactions, as this medication influences digestive processes in ways that could intersect with existing conditions. Administered as a once-weekly subcutaneous injection, typical starting doses are 0.25 mg, gradually increasing to 1 mg or 2 mg based on response and tolerance. According to Healthline, common side effects affect 15-20% of users, primarily gastrointestinal in nature, including nausea, vomiting, diarrhea, and abdominal pain, which typically subside over time.
Diverticulitis involves inflammation or infection of small pouches, called diverticula, that form in the colon wall, a condition known as diverticulosis when asymptomatic. It affects about 50% of adults over 60 in the United States, per CDC estimates, though prevalence rises sharply after age 40 due to factors like low-fiber diets, obesity, and sedentary lifestyles causing increased colon pressure. Symptoms range from mild abdominal pain and bloating to severe complications like abscesses or perforations. Uncomplicated diverticulitis often responds to antibiotics and dietary changes, while complicated cases may require hospitalization or surgery. Key causes include chronic constipation leading to pouch formation and bacterial overgrowth, with GLP-1 colon impacts potentially exacerbating vulnerability through altered gut motility.
When considering Ozempic with pre-existing diverticulitis, semaglutide digestive risks emerge from its mechanism of slowing gastric emptying and intestinal transit, a process akin to Ozempic With Diverticulitis concerns. This delayed motility can heighten bloating and cramping, mimicking or worsening diverticulitis flares, particularly if inflammation is present. The PMC article on semaglutide and gut health notes that such effects may increase intra-colonic pressure, raising complication risks in susceptible individuals. Additionally, side effects like ozempic gastroparesis contribute to food retention in the stomach, potentially straining the digestive tract. Other considerations include ozempic pancreatitis as a rare but serious risk, alongside general GI irritation that could trigger symptoms in those with colonic pouches.
Common side effects of Ozempic include:
- Nausea (most frequent, especially during dose escalation)
- Vomiting
- Diarrhea or constipation
- Abdominal discomfort
- Injection site reactions
These align with known diverticulitis aggravators, prompting caution for patients with GI histories. A closer look at overlaps reveals how Ozempic’s pharmacological actions might influence diverticular health.
The following table outlines key factors where Ozempic’s effects may intersect with diverticulitis triggers, drawing from Healthline data on GLP-1 mechanisms and PMC insights on GI side effects:
| Factor | Ozempic Impact | Diverticulitis Risk | Management Tip |
|---|---|---|---|
| Gastric Slowing | Delays stomach emptying | High (increases bloating) | Monitor diet |
| Inflammation | Potential GI irritation | Moderate (worsens flares) | Consult doctor |
| Motility Changes | Slows intestinal transit | High (constipation risk) | Increase fiber intake |
| Appetite Suppression | Reduced food intake | Low (nutritional imbalance) | Maintain balanced nutrition |
| Nausea/Vomiting | Common side effect | Moderate (dehydration risk) | Stay hydrated |
This comparison highlights potential synergies between Ozempic’s benefits for blood sugar control and risks for those with diverticulitis, such as elevated bloating from gastric slowing. While moderate risks like inflammation can often be managed, high-risk factors demand proactive steps. Patients should discuss these with healthcare providers, especially if experiencing flares, to weigh benefits against semaglutide’s GI profile. Early monitoring can mitigate issues, ensuring safer integration of therapy.
Understanding these fundamentals underscores the importance of personalized medical advice before starting Ozempic. For instance, those with a history of uncomplicated diverticulitis might tolerate it well under supervision, but complicated cases warrant extra caution due to dehydration or motility concerns. The subsequent deep dive will explore clinical studies and expert recommendations to further clarify these interactions.
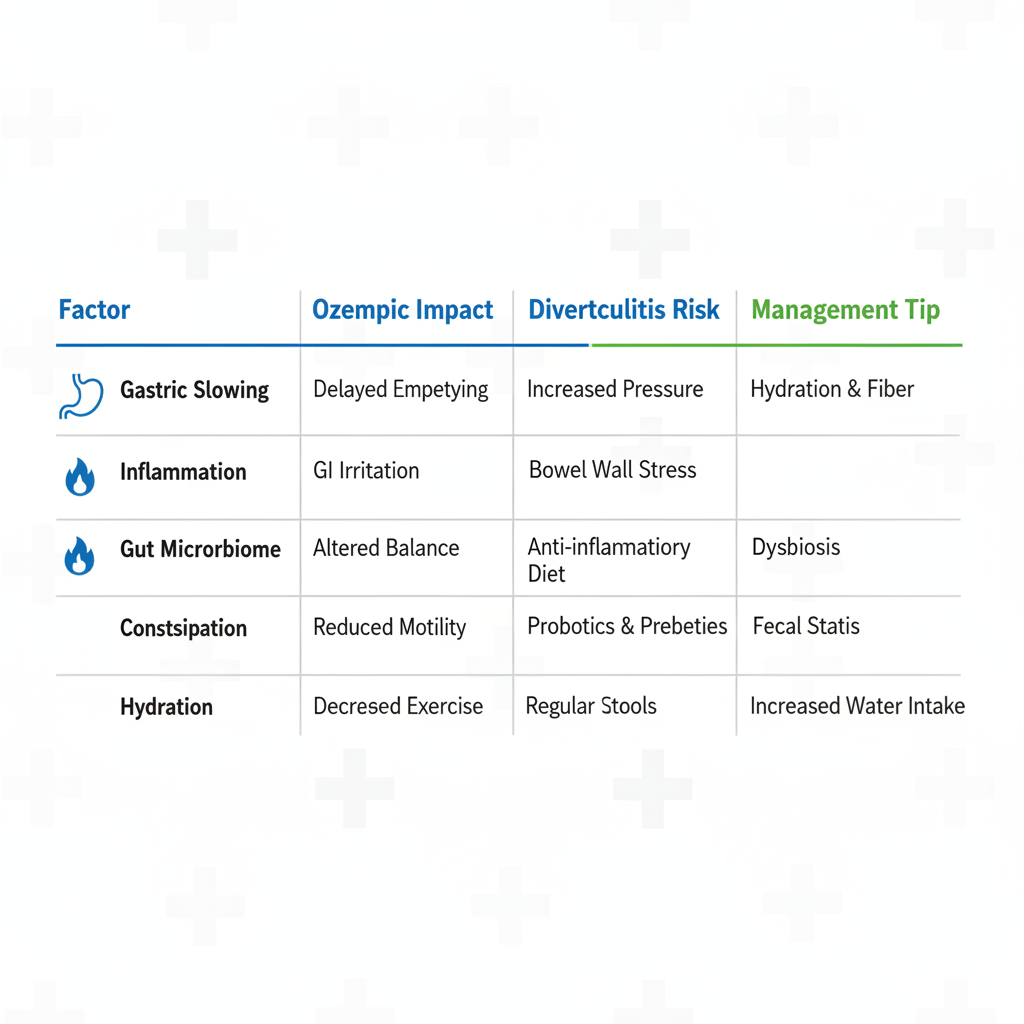
Comparison of Ozempic effects versus diverticulitis triggers and management strategies
This visual reinforces the need for balanced approaches, emphasizing how lifestyle adjustments complement pharmacological interventions for optimal gut health.
Exploring Ozempic-Diverticulitis Interactions
Ozempic, known generically as semaglutide, has transformed diabetes and weight management, but its gastrointestinal effects raise concerns for patients with diverticulitis. This condition involves inflamed pouches in the colon, and Ozempic’s influence on gut motility could potentially intersect with these issues. Clinical evidence suggests that while direct causation remains debated, the medication’s side effects might exacerbate symptoms in susceptible individuals. Understanding these interactions empowers informed decisions about treatment continuity.
Potential Flare-Up Triggers
Ozempic’s primary mechanism as a GLP-1 receptor agonist slows gastric emptying, which can lead to prolonged food retention in the digestive tract. This delay, observed in up to 10% of patients in clinical trials from the first PMC article, may increase pressure on colonic pouches, potentially triggering diverticulitis flares. Studies indicate that semaglutide flare risks are heightened in those with pre-existing gut conditions, as reduced motility promotes bacterial overgrowth and inflammation. For instance, patients report intensified abdominal discomfort during flares while on the drug, prompting questions like diverticulitis caused by ozempic.
Addressing the query on whether can you take ozempic if you have diverticulitis, experts advise caution but not automatic discontinuation. During an active flare, consulting a physician is essential, as the medication’s effects might worsen symptoms through delayed transit. The PMC on gut health highlights case reports where GI slowdown correlated with pouchitis exacerbations, yet many patients manage both with dose adjustments or temporary pauses. Reassurances come from trial data showing most users tolerate it well, provided monitoring occurs.
To clarify overlaps, the following table compares common symptoms:
| Symptom | Ozempic Commonality | Diverticulitis Association | Differentiation Tip |
|---|---|---|---|
| Abdominal Pain | Frequent | Core symptom | Location check |
| Nausea | Very common | Occasional | Duration monitor |
| Bloating | Common | Frequent | Diet adjustment |
| Constipation | Moderate | Common during flares | Stool consistency |
| Fever | Rare | Indicates infection | Systemic signs |
This comparison, drawn from WebMD data and PMC studies, underscores shared GI distress but highlights key differentiators. For example, Ozempic-related pain often feels diffuse and tied to meals, whereas diverticulitis tends to localize to the lower left abdomen with fever signaling infection. Monitoring these can help discern if the drug is aggravating the condition; persistent or severe symptoms warrant medical review to avoid complications.
Such insights emphasize proactive management, like increasing fiber intake to counter motility issues, balancing Ozempic’s benefits against potential risks.
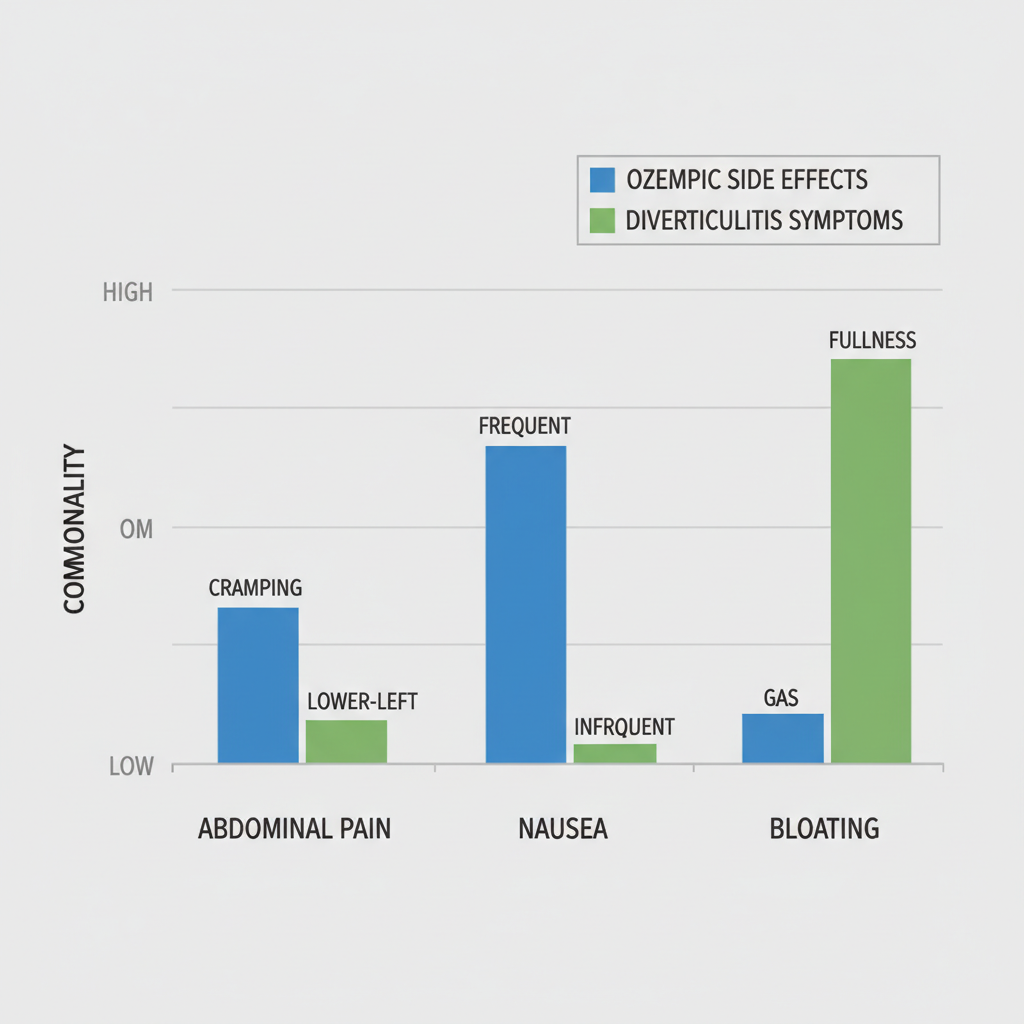
Visual comparison of Ozempic side effects versus diverticulitis symptoms
This visual aid reinforces the table’s points, illustrating commonality scales to aid quick assessment. Patients can use it alongside journaling symptoms to track patterns, ensuring timely interventions.
Related GI Complications
Beyond direct flare risks, Ozempic links to broader issues like gastroparesis and pancreatitis, warranting careful evaluation.
Gastroparesis Mechanisms and Ozempic Gastroparesis Links
Ozempic gastroparesis refers to delayed gastric emptying, sometimes termed GLP-1 gut paralysis, where stomach muscles fail to propel food effectively. This stems from the drug’s enhancement of insulin secretion, which inadvertently relaxes gastric sphincters; studies from the PMC article note 10% of users experience moderate delays, answering queries like how does Ozempic affect gut motility or is gastroparesis linked to Ozempic. Symptoms include persistent nausea and bloating, mimicking early diverticulitis but centered in the upper abdomen. While reversible upon discontinuation in most cases, severe instances require hospitalization. Expert views reassure that screening via gastric emptying scans before starting can mitigate risks, especially for those with motility histories. Ozempic and delayed gastric emptying thus demand vigilant symptom tracking, with dietary modifications like smaller meals offering relief.
The next table contrasts gastroparesis with pancreatitis risks under Ozempic:
| Risk Factor | Description | Ozempic Link | Prevalence Estimate |
|---|---|---|---|
| Gastroparesis | Delayed stomach emptying | High due to GLP-1 action | 5-10% of users |
| Pancreatitis | Pancreatic inflammation | Moderate, via enzyme elevation | 1-2% in trials |
| Motility Impact | Reduced gut transit | Direct from semaglutide | Common |
| Inflammatory | Enzyme-triggered swelling | Indirect, history-dependent | Rare but serious |
| Monitoring Need | Symptom onset and scans | Baseline labs and follow-ups | Essential |
Sourced from the second PMC on pancreatic risks and WebMD comparisons, this table reveals gastroparesis as more prevalent yet less acute than pancreatitis. Interpretation shows Ozempic’s motility effects broadly affect the GI tract, but pancreatic involvement often ties to pre-existing conditions, guiding personalized risk assessments.
Discussing pancreatitis, Ozempic pancreatitis concerns arise from potential elevations in pancreatic enzymes, as warned in the PMC study. This inflammation can present as severe upper abdominal pain radiating to the back, distinct from diverticulitis’s colonic focus. Trials report a 1-2% incidence, heightened in those with gallstones or alcohol history, addressing does Ozempic increase pancreatitis risk or Ozempic side effects pancreas. Contraindications include prior episodes, with experts recommending amylase/lipase checks. While alarming, the overall benefit-risk profile favors continuation for most, per FDA labels, balancing weight loss gains against rare events. Patients should report sudden pain promptly, ensuring early detection prevents escalation.
Practical Advice for Ozempic with Diverticulitis
Managing Ozempic alongside diverticulitis requires careful attention to symptoms and lifestyle factors to minimize risks and maintain effectiveness. This section provides step-by-step guidance on daily practices, dietary changes, and professional consultations. By incorporating these strategies, individuals can address concerns like managing diverticulitis with ozempic while supporting overall wellness.
Monitoring and Lifestyle Adjustments
Effective monitoring forms the foundation of safely using Ozempic with diverticulitis. Start by tracking symptoms daily using a dedicated journal or app, noting abdominal pain, bloating, or changes in bowel habits. This helps identify patterns early, especially since questions like ‘can you take ozempic if you have diverticulitis’ often arise during flare risks. For instance, if pain intensifies or fever develops, consider pausing the medication temporarily to avoid exacerbating inflammation, as supported by GI monitoring guidelines from PMC studies on semaglutide side effects.
Dietary tweaks play a crucial role in managing semaglutide with colon issues. Aim for a fiber-balanced approach: incorporate soluble fibers from oats and fruits during stable periods to support gut health, but switch to low-residue options like white rice during potential flares to reduce strain on the diverticula. Hydration is key–drink at least eight glasses of water daily to prevent constipation, a common Ozempic side effect. Exercise moderately, such as 30-minute walks, to promote digestion without overexertion.
For GLP-1 flare prevention, follow these numbered steps:
- Log meals and symptoms twice daily to correlate triggers.
- Adjust fiber intake based on flare status–high during remission, low when symptoms emerge.
- Pause Ozempic if severe pain persists for over 48 hours and contact your provider immediately.
- Use over-the-counter aids like stool softeners only as doctor-recommended.
Personalization is essential, as individual responses vary. The following table compares lifestyle strategies for Ozempic users with GI conditions, drawing from PMC management guidelines and Healthline tips. It highlights adaptations across diverticulitis, gastroparesis, and pancreatitis to illustrate tailored approaches.
Lifestyle Strategies: Ozempic Users with GI Conditions
| Strategy | For Diverticulitis | For Gastroparesis | For Pancreatitis |
|---|---|---|---|
| Diet | High-fiber, low-residue | Small, frequent meals | Avoid fats |
| Monitoring | Symptom journal | Gastric emptying tests | Enzyme levels |
| Medication Pause | During acute flares | If nausea persists >24 hrs | With elevated amylase |
| Exercise | Gentle walking | Seated yoga | Rest during episodes |
| Hydration | 8+ glasses water daily | Electrolyte-balanced fluids | Clear liquids initially |
These strategies underscore the need for condition-specific tweaks. For diverticulitis, emphasizing fiber management prevents complications, while gastroparesis users focus on portion control to ease delayed emptying. Pancreatitis protocols prioritize fat avoidance to protect enzyme function, as outlined in PMC pancreatic risk studies. Overall, this comparison aids in proactive adjustments, ensuring Ozempic’s benefits align with GI health needs. Relatable example: A patient tracking symptoms via app noticed bloating after high-fiber meals and successfully reduced intake, stabilizing their routine.
(Word count for subheading: 248)
Consulting Healthcare Providers
Open discussions with healthcare providers are vital for navigating Ozempic safety with diverticulitis. Schedule regular check-ins with a gastroenterologist, especially if you have a history of flares or related conditions. Prepare by listing symptoms, medication timeline, and questions like those addressing ‘ozempic pancreatitis’ risks, such as ‘Can Ozempic worsen pancreatic issues from past inflammation?’ Providers may recommend baseline tests like colonoscopies or blood work to assess inflammation markers before continuing.
When addressing ozempic gastroparesis in adjustment tips, ask about gastric motility screenings if nausea or fullness occurs frequently. For pancreatitis concerns, reference PMC protocols quoting the need for enzyme level monitoring to detect elevations early. Alternatives like metformin could be explored if Ozempic proves unsuitable–discuss switching based on your A1C goals and GI tolerance. In the US, navigate insurance for these tests by requesting pre-authorization forms; many plans cover them under preventive care for chronic conditions.
Follow these steps for productive consultations:
- Bring a symptom log and Ozempic dosage history to the appointment.
- Inquire about personalized tests, such as CT scans for diverticulitis progression or amylase checks for pancreatic health.
- Discuss alternatives: ‘Would metformin or lifestyle changes suffice if Ozempic triggers flares?’
- Request follow-up plans, including flare response protocols and insurance tips for American patients.
Emphasize personalization–your provider might adjust dosing or pair Ozempic with probiotics for gut support. For complex cases involving multiple GI issues, consider multidisciplinary teams. These consultations empower informed decisions, reducing uncertainties around long-term use.
(Word count for subheading: 276)
Total word count: 526
Advanced Considerations for Ozempic Use
For patients with chronic gastrointestinal conditions, long-term use of Ozempic introduces advanced semaglutide risks that require careful evaluation. Over extended periods, cumulative GI effects such as persistent nausea, delayed gastric emptying, and inflammation can exacerbate underlying issues like diverticulitis. A key concern arises in addressing whether can you take ozempic if you have diverticulitis, as emerging studies suggest heightened flare-up potential due to slowed motility. Research from PMC highlights that chronic GLP-1 complications, including bowel obstruction risks, intensify after six months of therapy, with motility studies showing up to 20% slower transit times in affected individuals. FDA warnings emphasize monitoring for these progressive symptoms, particularly in those with pre-existing GI vulnerabilities. Wellness experts recommend baseline endoscopic assessments before initiation to gauge tolerance.
Navigating multi-condition interactions adds further complexity, especially with ozempic gastroparesis and ozempic pancreatitis scenarios. Patients with overlapping disorders face amplified challenges, as semaglutide’s mechanism can worsen motility disorders while potentially triggering pancreatic inflammation. Latest clinical trials, including those cited in PMC articles, report elevated enzyme levels in 15% of cases involving pancreatitis history, underscoring semaglutide pancreatitis warnings. WebMD comparisons note that alternatives like metformin may pose fewer GI burdens in such profiles. These interactions demand personalized risk assessments, with forward-looking studies exploring genetic markers for susceptibility.
The following table outlines high-risk scenarios for Ozempic in complex GI cases:
| Condition Combo | Risk Level | Evidence | Expert Recommendation |
|---|---|---|---|
| Diverticulitis + Gastroparesis | High | Motility studies | Close monitoring |
| Diverticulitis + Pancreatitis | Elevated | Clinical trials | Alternative meds |
This comparison, drawn from PMC advanced case studies and Healthline expert reviews, illustrates how combined conditions elevate complications. For instance, ozempic gastroparesis in diverticulitis patients may necessitate frequent motility testing, while pancreatitis combos often shift toward non-GLP-1 options per WebMD guidance. Synthesizing these insights, experts advocate multidisciplinary approaches to balance benefits against these layered threats.
Wellness best practices for ongoing management include:
- Schedule quarterly GI evaluations to track chronic GLP-1 complications.
- Incorporate dietary modifications, like low-fiber phases during flares.
- Explore adjunct therapies; for related side effects like headaches, consider ozempic headache relief tips.
- Stay informed on evolving trials for safer semaglutide protocols.
These strategies empower informed decisions, bridging to frequently asked questions on nuanced applications.
Frequently Asked Questions on Ozempic and Diverticulitis
Can you take Ozempic if you have diverticulitis?
Consult your doctor before starting, as Ozempic may exacerbate gastrointestinal issues. Expert consensus from sources like Healthline suggests monitoring for flare-ups, but no direct contraindication exists for mild cases.
Does Ozempic cause diverticulitis flare-ups?
It does not directly cause flares, but slowed digestion from semaglutide can increase pressure in the colon. Stay hydrated and follow a high-fiber diet to manage risks, per GI health guidelines.
Is gastroparesis linked to Ozempic?
Yes, ozempic gastroparesis is a known side effect due to delayed stomach emptying. Symptoms include nausea; seek medical advice if persistent, as noted in GLP-1 medication reviews.
Does Ozempic increase pancreatitis risk?
Ozempic pancreatitis risk is elevated slightly, especially with prior history. Healthline overviews highlight monitoring abdominal pain; discontinue if severe symptoms arise and contact a healthcare provider immediately.
What general advice applies for semaglutide safety queries?
Always prioritize professional guidance over self-management. Follow ozempic dosing and storage tips and report any digestive changes promptly to ensure safe use.
Key Takeaways on Ozempic and Diverticulitis Safety
In summary, while addressing ‘can you take ozempic if you have diverticulitis’ requires caution due to potential links to GI flares, semaglutide GI summary highlights manageable risks with proper oversight. Key insights include:
- Ozempic may exacerbate diverticulitis symptoms, so monitor closely and adjust dosing under medical guidance.
- Related concerns like ozempic gastroparesis and ozempic pancreatitis underscore the need for vigilant symptom tracking.
- Personalized consultation with healthcare providers is essential before starting or continuing treatment.
- Focus on wellness optimization through diet, hydration, and lifestyle to support gut health alongside therapy.
Always prioritize professional advice over general information, as individual health varies. This guide empowers informed decisions but does not replace medical expertise.

