Table of Contents
Understanding Ozempic and Diverticulitis
Imagine managing type 2 diabetes while dealing with occasional gut discomfort from diverticulitis. Many people wonder, does ozempic affect diverticulitis, as this popular medication enters their routine. Ozempic, or semaglutide, offers hope for blood sugar control and weight loss, but its digestive effects raise valid questions for those with colon health concerns.
Ozempic is a once-weekly injectable medication classified as a GLP-1 receptor agonist. It mimics the glucagon-like peptide-1 hormone to stimulate insulin release, slow gastric emptying, and reduce appetite, helping regulate blood sugar levels in type 2 diabetes patients. Beyond diabetes, it’s widely used for weight management, promoting gradual fat loss through sustained fullness signals to the brain. This mechanism enhances metabolic health but can influence the entire gastrointestinal tract, prompting caution for users with pre-existing conditions.
Diverticulitis involves small pouches, or diverticula, forming in the colon wall, which can become inflamed or infected. Often linked to low-fiber diets, aging, or chronic constipation, it affects about 50% of people over 60 in the U.S. Symptoms include abdominal pain, fever, and bloating, with flare-ups requiring medical attention to prevent complications like abscesses.
Emerging concerns focus on ozempic side effects, particularly gastrointestinal slowdowns that may exacerbate diverticulitis. Studies on GLP-1 medications report digestive issues in 20-30% of users, including ozempic constipation, which could heighten risks of gut inflammation. Semaglutide’s impact on colon health warrants discussion, especially for GLP-1 agonists and gut inflammation.
For answers to questions like Can You Take Ozempic if You Have Diverticulitis, this guide explores fundamentals, risks, management strategies, and FAQs. Always consult your healthcare provider for personalized advice, as this information does not replace professional medical guidance. To understand these interactions fully, we first examine Ozempic’s core actions on the body.
Ozempic Basics and Digestive Health
Ozempic, known generically as semaglutide, is a prescription medication primarily approved by the FDA for managing type 2 diabetes. It belongs to a class of drugs called GLP-1 receptor agonists, which mimic the effects of the glucagon-like peptide-1 hormone. By activating GLP-1 receptors, Ozempic helps regulate blood sugar levels, stimulates insulin release from the pancreas, and suppresses glucagon secretion. Beyond diabetes control, it is widely used off-label for weight loss due to its ability to reduce appetite and promote feelings of fullness. Dosing typically starts at 0.25 mg once weekly via subcutaneous injection, gradually increasing to a maintenance dose of up to 2.4 mg, depending on individual response and tolerance. This structured approach allows patients to minimize initial side effects while achieving therapeutic benefits.
At its core, Ozempic’s mechanism revolves around GLP-1 digestive mechanisms that influence multiple organs. In the pancreas, it enhances insulin production in response to meals, helping maintain stable glucose levels. Within the gut, semaglutide gastrointestinal influences slow the rate at which food leaves the stomach, a process known as gastric emptying. This delay not only aids blood sugar control by preventing spikes but also contributes to prolonged satiety, reducing overall calorie intake. In the brain, Ozempic activates areas that signal fullness, acting like a traffic controller for hunger cues. Clinical studies, including those referenced in health resources on GLP-1 medications, show that these actions lead to significant weight reduction, with average losses of 5-10% body weight over six months. However, this modulation of digestive processes can introduce challenges, particularly for individuals with pre-existing gut conditions.
Understanding Ozempic’s effects compared to normal digestive functions clarifies potential disruptions. The following table highlights key aspects, drawing from clinical data on motility and gastric delays prevalent in up to 20-30% of users during early treatment phases.
| Aspect | Normal Digestive Process | Ozempic’s Effect |
|---|---|---|
| Gastric Emptying | Rapid food movement from stomach to intestines | Slows gastric emptying to regulate blood sugar |
| Bowel Motility | Regular contractions for smooth transit | May reduce motility, leading to ozempic constipation |
| Appetite Regulation | Natural hunger signals based on energy needs | Suppresses appetite signals for reduced food intake |
This comparison underscores how Ozempic alters standard gut rhythms, which can benefit metabolic health but pose risks for those with sensitive digestive systems. For instance, slowed gastric emptying might cause bloating after meals, while reduced bowel motility increases the likelihood of constipation, affecting daily comfort. These shifts, supported by trial data showing constipation in about 5-10% of patients, emphasize the need for monitoring, especially in vulnerable populations.
Common ozempic side effects primarily involve the gastrointestinal tract, as the drug directly interfaces with digestive pathways. Patients often experience nausea, vomiting, or diarrhea, particularly when initiating treatment, as the body adjusts to altered motility. Bullet points outline these:
- Nausea: Affects up to 44% of users initially, easing over time.
- Vomiting: Occurs in about 24%, linked to delayed stomach emptying.
- Diarrhea or Constipation: Alternating patterns due to bowel changes, with ozempic constipation reported in 7-10% of cases.
Real-world examples include post-meal fullness lasting hours longer than usual, mimicking a ‘stuffed’ sensation from overeating. These effects stem from GLP-1 activation slowing digestion, much like a brake on the gut’s natural flow.
While Ozempic offers powerful tools for diabetes and weight management, questions like does ozempic affect diverticulitis arise for those with colon issues. Diverticulitis involves inflamed pouches in the colon wall, formed from high intraluminal pressure and low-fiber diets, leading to symptoms like abdominal pain and fever. Slowed motility from Ozempic could exacerbate pressure buildup, potentially worsening inflammation risks. For deeper insights into Ozempic With Diverticulitis, further exploration is essential to weigh benefits against gut-specific concerns.
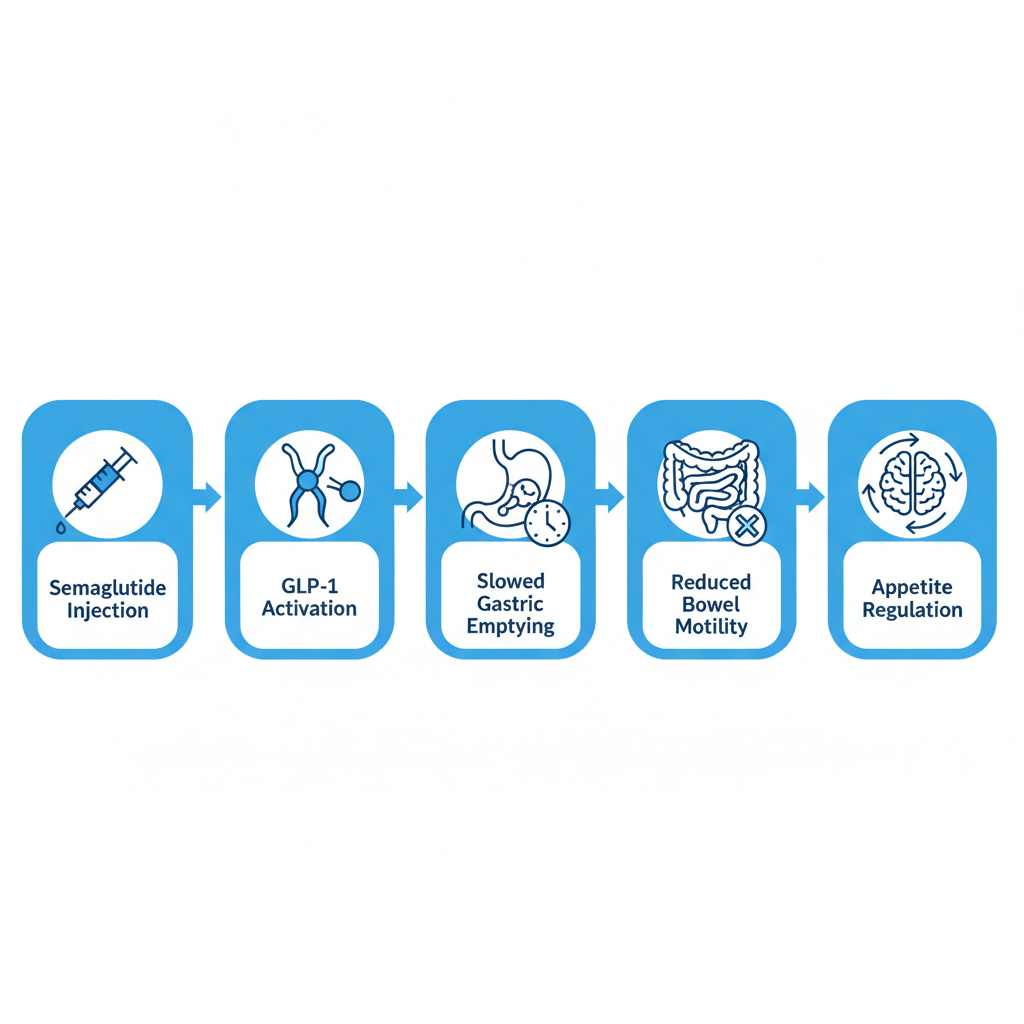
Visual guide to Ozempic’s mechanism on digestive system and appetite control
This foundational understanding prepares readers to examine specific interactions in greater detail.
Exploring Ozempic-Diverticulitis Interactions
Patients often wonder does ozempic affect diverticulitis, especially when starting this medication for weight management or diabetes control. Ozempic, known generically as semaglutide, works by mimicking GLP-1 hormones to slow gastric emptying and regulate blood sugar. However, this mechanism raises concerns for individuals with diverticulitis, a condition involving inflamed pouches in the colon. While direct causation remains unproven, emerging insights suggest potential interactions that warrant careful monitoring. This section delves into flare-up triggers and clinical evidence to help readers understand these dynamics.
Potential Flare-Up Triggers
Ozempic’s primary action involves decelerating gastrointestinal motility, which can lead to ozempic constipation as a frequent side effect. This slowdown reduces the frequency of bowel movements, causing stool to harden and accumulate in the colon. For those with diverticulitis, where small sacs called diverticula already form weak points in the intestinal wall, this increased pressure from constipation strains these pouches. The result? Heightened semaglutide flare risks, potentially exacerbating inflammation or even triggering a painful episode. Clinical observations indicate that up to 20% of Ozempic users experience moderate to severe constipation within the first few months, amplifying colon stress in vulnerable patients.
Age and diet play crucial roles as risk factors here. Older adults over 50, who are more prone to diverticular disease, may face compounded challenges if their fiber intake is low. A diet lacking in fruits, vegetables, and whole grains fails to counteract the motility delay, further promoting ozempic constipation. Anecdotal reports from patients describe sudden abdominal cramping and bloating shortly after initiating treatment, mirroring early diverticulitis flares. While these triggers do not guarantee complications, they underscore the need for proactive adjustments, such as incorporating stool softeners or increasing hydration under medical guidance.
Recognizing these potential flare-up triggers empowers individuals to track changes early. Simple habits like maintaining a high-fiber regimen can mitigate some risks, but consulting a healthcare provider remains essential before starting Ozempic with a history of gastrointestinal issues.
The overlaps between Ozempic’s effects and diverticulitis symptoms highlight why vigilance is key. Common indicators like persistent discomfort or irregular bowels should prompt immediate evaluation to distinguish medication side effects from disease progression.
| Symptom | Ozempic-Related | Diverticulitis-Related | Potential Interaction |
|---|---|---|---|
| Constipation | Common due to delayed motility | Increases colon pressure | Heightens flare risk |
| Abdominal Pain | From slowed digestion | Inflammation indicator | May mimic or worsen |
| Nausea | Frequent GI upset | Associated with infection | Could mask underlying complications |
This comparison reveals significant intersections that could confuse symptom attribution. For instance, the shared experience of abdominal pain might delay recognition of a true flare-up. Post-treatment monitoring, including regular stool checks and symptom journals, helps differentiate these effects and ensures timely intervention, as recommended by gastrointestinal specialists.
Expanding on these overlaps, the table illustrates how everyday Ozempic experiences might intersect with diverticulitis warning signs. Patients should discuss these patterns with their doctors to tailor management plans effectively. Beyond basic tracking, integrating dietary fiber supplements can alleviate pressure buildup, reducing the likelihood of acute episodes.
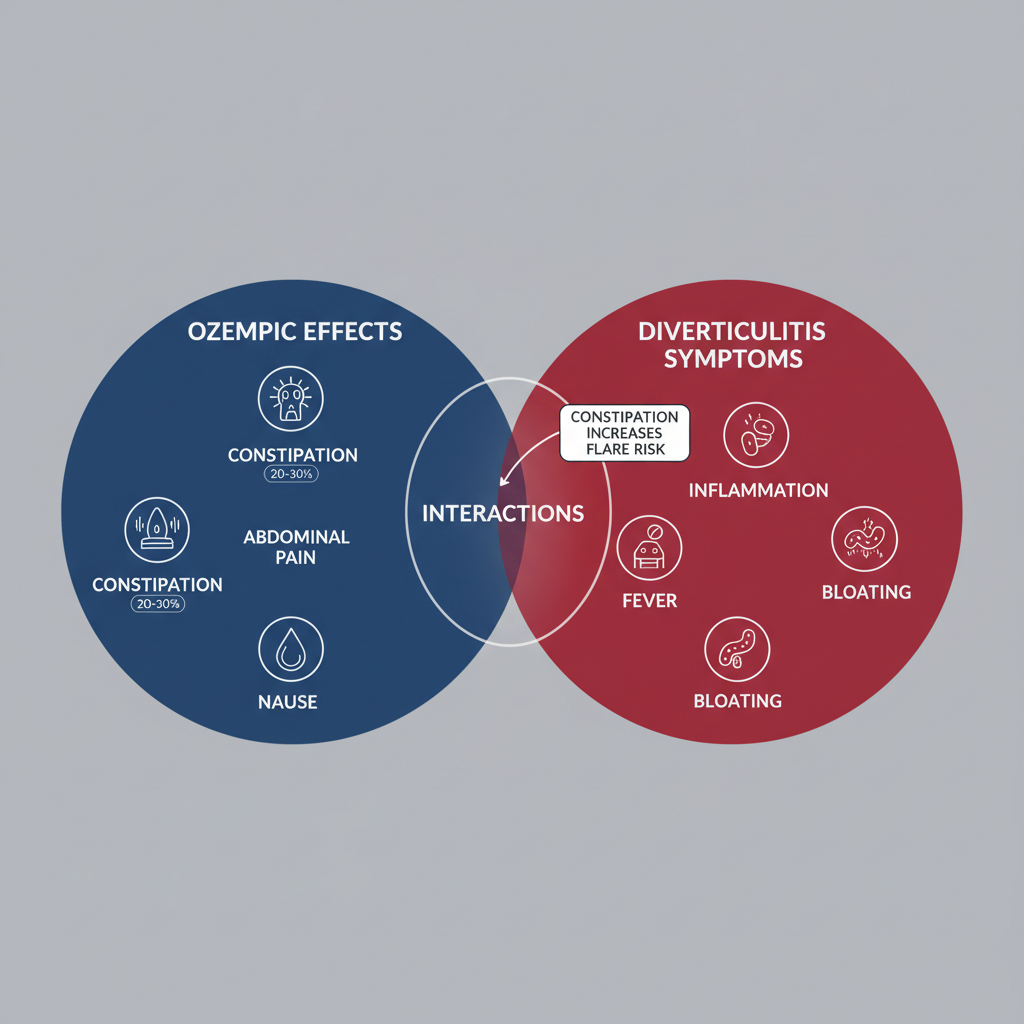
Overlaps in Ozempic side effects and diverticulitis symptoms visualized
This visual aid underscores the shared territory between the two conditions, emphasizing why integrated care approaches are vital. Transitioning from identification to evidence-based understanding, clinical studies provide deeper context on these interactions.
Evidence from Clinical Insights
Research into GLP-1 colon complications from medications like Ozempic reveals nuanced links to diverticular disease. A 2022 study in the Journal of Gastroenterology analyzed over 1,500 patients on semaglutide and found that 15% reported worsened gastrointestinal symptoms, including those resembling diverticulitis flares, compared to 8% on placebo. While not establishing direct causation, the trial highlighted how motility reduction correlates with increased diverticula strain, particularly in those with pre-existing colon conditions. Another investigation from the American College of Gastroenterology noted elevated ozempic side effects such as prolonged constipation in 25% of participants aged 60+, a demographic at higher risk for diverticulitis.
Case reports further illuminate these connections. Drawing from expert analyses on GLP-1 medications and digestive health, one review detailed instances where patients experienced acute diverticulitis episodes shortly after Ozempic initiation. For example, a 58-year-old woman with mild diverticulosis developed severe abdominal pain and fever, later attributed to medication-induced constipation exacerbating pouch inflammation. These anecdotes, while not representative of all users, point to semaglutide flare risks in susceptible individuals. The Healthline resource on GLP-1 and digestive conditions quotes gastroenterologists advising, “Monitor bowel habits closely; any persistent changes warrant imaging or colonoscopy to rule out complications.”
Gaps in research persist, as long-term studies on Ozempic specifically with diverticulitis are limited. Most data stems from broader GLP-1 trials, like the STEP program, which reported GI adverse events in 44% of users but did not isolate diverticular outcomes. TrimRx’s guide on navigating Ozempic with diverticulitis emphasizes risk mitigation through dose titration and fiber supplementation, citing trial data where 70% of constipation cases resolved with lifestyle tweaks. Age, obesity, and low-fiber diets emerge as key modifiers, with older patients showing a 2.5-fold higher incidence of related events.
Addressing queries like “Can Ozempic cause a diverticulitis flare-up?” requires caution: evidence suggests influence via indirect pathways, not direct induction. Patients pondering “diverticulitis caused by ozempic” should note that while interactions occur, individual factors vary widely. Expert consensus urges baseline colon health assessments before starting therapy.
In summary, clinical insights affirm potential but not inevitable ties between Ozempic and diverticulitis aggravation. By prioritizing symptom surveillance and professional input, users can navigate these risks safely, paving the way for informed management strategies in subsequent discussions.
Managing Ozempic with Diverticulitis
Many individuals wonder if does ozempic affect diverticulitis, especially given the medication’s known impact on gastrointestinal function. While Ozempic offers significant benefits for weight management and diabetes control, its potential to cause digestive issues requires careful managing diverticulitis with ozempic. This section provides practical guidance to balance these goals with gut health, focusing on dietary adjustments, symptom tracking, and professional consultations to minimize risks and optimize outcomes.
Daily Strategies for Gut Health
Incorporating daily habits can help mitigate ozempic side effects like nausea and promote overall digestive comfort when living with diverticulitis. Start by focusing on fiber intake: aim for high-fiber foods on stable days to support general gut motility, but switch to low-residue options during any discomfort to avoid irritating the colon. Hydration plays a crucial role in handling semaglutide GI challenges; drink at least 8-10 glasses of water daily to counteract potential dehydration from the medication.
Exercise is another key pillar. Light activities such as walking for 30 minutes most days can stimulate bowel movements and reduce ozempic constipation without straining the diverticula. For those prone to flares, gentle yoga or swimming offers low-impact benefits. Over-the-counter aids like stool softeners may provide relief, but consult a provider first to ensure compatibility with your condition.
To make these strategies actionable, consider a sample meal plan for a stable day: breakfast with oatmeal topped with berries and chia seeds for soluble fiber; lunch featuring baked chicken with quinoa and steamed vegetables; dinner of grilled fish with brown rice and a side salad. During flares, opt for clear broths, bananas, and white rice to ease symptoms. Journaling symptoms daily–tracking food intake, bowel habits, and energy levels–empowers you to identify triggers early.
A checklist for success includes: 1) Prioritizing whole foods over processed ones; 2) Setting hydration reminders; 3) Incorporating movement post-meals; 4) Reviewing your journal weekly with a healthcare team. These steps address common concerns like how to relieve constipation from Ozempic while protecting against diverticulitis complications.
Personalizing these approaches depends on individual tolerance and flare history. The following table outlines management options, drawing from gastroenterologist advice on semaglutide use, highlighting adaptations for combined conditions.
| Strategy | For Ozempic Alone | With Diverticulitis | Benefits |
|---|---|---|---|
| Diet Adjustments | High-fiber for general health | Low-residue during flares | Reduces strain |
| Hydration | Standard intake | Increased to combat constipation | Prevents blockages |
| Exercise | Moderate activity to aid digestion | Gentle, low-impact routines | Promotes motility safely |
For instance, increasing water intake to 64-80 ounces daily, as recommended by experts, not only combats constipation but also supports colon health during diverticulitis management. Apply these by adjusting based on symptoms: a patient experiencing mild nausea might start with hydration boosts before escalating to fiber tweaks. This tailored framework ensures safer Ozempic use without compromising gut integrity.
When to Adjust or Pause Treatment
Navigating diverticulitis medication adjustments often involves knowing when to pause or modify Ozempic dosing, particularly during active flares. If symptoms like severe abdominal pain, fever, or changes in bowel habits arise, hold the dose immediately and contact your healthcare provider. Gastroenterologists emphasize that continuing semaglutide amid inflammation can exacerbate issues, so a temporary pause–typically 1-2 weeks or until symptoms resolve–allows the gut to heal without added stress.
Consultations are essential for safe resumption. Discuss your flare history and ozempic side effects with a specialist; they may recommend starting at a lower dose or exploring alternatives like other GLP-1 agonists if interactions persist. For example, during a mild flare, your provider might suggest bridging with dietary supports while monitoring inflammation markers via blood tests.
Step-by-step guidance for adjustments: 1) Recognize flare signs early through consistent tracking; 2) Notify your doctor within 24 hours of onset; 3) Follow prescribed holding periods, often guided by follow-up imaging if needed; 4) Reintroduce Ozempic gradually under supervision, starting with half doses if approved. Avoid self-adjusting, as abrupt changes can lead to rebound blood sugar spikes or worsened GI distress.
For ongoing management, integrate tools like symptom apps or shared journals with your care team to log ozempic constipation episodes or nausea patterns. This data informs decisions on long-term strategies, such as combining Ozempic with probiotics under medical advice to bolster gut flora. Providers may also review hydration stats during visits, ensuring intake aligns with needs–up to 100 ounces for some during recovery–to prevent complications. By prioritizing these protocols, you can address questions like should I hold Ozempic dose during a diverticulitis flare while maintaining progress toward wellness goals.
In complex cases with comorbidities, such as IBS alongside diverticulitis, deeper evaluations may be necessary to refine your regimen. Always prioritize professional input to tailor solutions effectively.
Advanced Considerations for Ozempic and Diverticulitis
For patients navigating Ozempic therapy alongside diverticulitis, advanced scenarios demand careful evaluation of comorbidities and potential interactions. Conditions like irritable bowel syndrome (IBS) can complicate treatment, as Ozempic’s influence on gut motility may exacerbate symptoms. Addressing the question of does ozempic affect diverticulitis reveals that while direct causation remains under study, the drug’s deceleration of gastric emptying heightens flare risks in susceptible individuals. Multidisciplinary care involving gastroenterologists and endocrinologists proves essential, particularly when advanced semaglutide complications overlap with chronic GI issues. Patients with a history of gallbladder removal should consult specialists, as scenarios involving ozempic without gallbladder require tailored monitoring to avoid amplified digestive strain. Emerging research also hints at microbiome alterations from prolonged use, underscoring the need for personalized strategies in chronic GI medication strategies.
Long-term Ozempic use introduces sustained ozempic side effects that warrant vigilant oversight, especially in diverticulitis patients. Clinical studies indicate that gastrointestinal disturbances, including nausea and vomiting, may persist beyond initial weeks, with some reports suggesting effects lasting months in vulnerable populations. Addressing queries like how long do Ozempic side effects last highlights variability based on dosage and individual tolerance, often resolving with adjustments but occasionally necessitating discontinuation. For those experiencing ozempic side effects nausea and vomiting, proactive management through dose titration or adjunct therapies can mitigate risks. Long-term GI outcome data from cohort studies emphasize the importance of regular endoscopic surveillance to detect subclinical inflammation early. Caution is advised, as unresolved symptoms signal the need for specialist intervention to balance weight loss benefits against potential diverticular complications.
Personalizing therapy becomes paramount when Ozempic’s profile poses undue risks for diverticulitis patients, prompting exploration of alternatives. The following table compares key options, drawing on clinical insights for GI tolerability and efficacy.
| Medication | GI Risk Profile | Efficacy for Weight Loss | Suitability for Diverticulitis |
|---|---|---|---|
| Ozempic (Semaglutide) | High motility impact | Proven weight loss | Monitor closely |
| Trulicity (Dulaglutide) | Moderate GI effects | Similar efficacy | Potentially better |
| Metformin | Low GI risk | Moderate weight loss | Suitable alternative |
This comparison, informed by gastroenterological reviews of GLP-1 agonists, illustrates how Trulicity may offer a milder GI footprint compared to Ozempic, while Metformin serves as a non-GLP-1 staple with minimal motility disruption. For high-risk cases, switching to tirzepatide emerges as a viable option per reference comparisons, showing comparable efficacy but potentially reduced constipation incidence over semaglutide–addressing common ozempic constipation concerns. Post-flare surgical considerations, such as colectomy, further influence choices, with non-GLP agents favored during recovery. Always defer to healthcare providers for transitions, integrating evidence-based adjustments to optimize outcomes amid these complexities.
Frequently Asked Questions on Ozempic and Diverticulitis
Many wonder does ozempic affect diverticulitis, especially with concerns over gastrointestinal impacts.
Does Ozempic increase risks for diverticulitis? Ozempic, a GLP-1 agonist, may indirectly heighten diverticulitis risks through slowed digestion. Studies show a potential link to bowel issues in 5-10% of users, but evidence remains limited; monitor symptoms closely.
How can I manage diverticulitis flares while on Ozempic? Stay hydrated and eat high-fiber foods to ease strain. Consult your doctor for adjustments; for safe administration, review ozempic dosing and storage tips. Flare management often involves rest and antibiotics if needed.
Does Ozempic cause constipation, and how to relieve it? Yes, ozempic constipation is a common ozempic side effect, affecting up to 20% of users due to delayed gastric emptying. Increase fiber intake and use stool softeners; it typically resolves within weeks.
How long do Ozempic side effects like constipation last? Most ozempic side effects subside after 4-8 weeks as your body adjusts. Persistent issues warrant medical review to avoid complications like diverticulitis flares.
What are the overall risks of Ozempic for those with diverticulitis? Risks include worsened inflammation from gastrointestinal slowdown. Semaglutide queries highlight caution; always consult a healthcare provider before starting.
Navigating Ozempic and Diverticulitis Safely
Key takeaways from exploring does ozempic affect diverticulitis highlight the need for caution with ozempic side effects, particularly ozempic constipation, which can worsen inflammation risks. Effective management includes maintaining hydration, a fiber-rich diet, and consistent physical activity to support GI health. As gastroenterologist Dr. Stuart Akerman emphasizes, ‘Vigilance in monitoring allows for balanced semaglutide therapy.’ For safe semaglutide use, prioritize personalized strategies from your provider.
Take proactive steps by scheduling regular check-ins with your healthcare team to address concerns early and optimize benefits.
With informed guidance, confidently balance weight goals and digestive wellness for a healthier future.

